2022 Market Trends for Home Health and Personal Care
Home and Community Based Care is changing in 2022. States are starting their official rollout, compliance regulations are becoming more robust, and home health agencies are just entering the EVV space. Whether you’ve been EVV compliant for a while or you’re just entering the world of Electronic Visit Verification compliance, we have outlined EVV trends for the home health, self-direction, and personal care markets.
A Shift Away From Institutional Care
Since the start of the COVID-19 Pandemic in 2020, we have started to see this shift away from institutional long-term care accelerate, as more studies prove that our most vulnerable loved ones are safer when at home.
According to the Medicaid Innovation Accelerate Program, (IAP), growth in home and community services continues, as the 1915 C waiver programs (many of which are home-based services) grew by 7.9% between 2014 and 2015. And grew again at 8.2% from 2015 to 2016.
 The Kaiser Family Foundation estimates that Medicaid home and community-based service spending will come to $114 billion in fiscal year 2021 before any increase from the American Rescue Plan Act.
The Kaiser Family Foundation estimates that Medicaid home and community-based service spending will come to $114 billion in fiscal year 2021 before any increase from the American Rescue Plan Act.
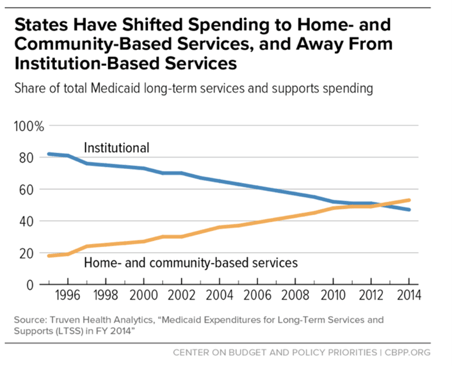
"We've seen people more and more wanting to receive long-term care in their homes as opposed to institutions." Figure 1, left, shows how home and community-based services have eclipsed spending on institutional services--much of this eclipse has been driven by patient preference. As the United States population ages, more patients are choosing to age in the comfort of their own homes.
From a cost-reduction perspective, the shift away from institutional care is inevitable. Time and again home-based care has proven to be cost-effective and most comfortable for patients who need long-term care.
Shift Towards Managed Care
Over the last decade, a shift towards managed care states so drastically increased their use of managed care to deliver Medicaid or CHIP benefits.
 According to Medicaid, "Managed Care is a health care delivery system organized to manage cost, utilization, and quality. Medicaid managed care provides for the delivery of Medicaid health benefits and additional services through contracted arrangements between state Medicaid agencies and managed care organizations (MCOs) that accept a set per member per month (capitation) payment for these services."
According to Medicaid, "Managed Care is a health care delivery system organized to manage cost, utilization, and quality. Medicaid managed care provides for the delivery of Medicaid health benefits and additional services through contracted arrangements between state Medicaid agencies and managed care organizations (MCOs) that accept a set per member per month (capitation) payment for these services."
Managed Care is now becoming the dominant delivery system in both programs, as of July 2018, About 34 million individuals were enrolled in Medicaid Managed Care, which is about 69% of total Medicaid enrollment. In fiscal year 2018, total federal and state Medicaid managed care expenditures were $296 billion, which is about 50% of total Medicaid. In 31 states, about 79% of CHIP children were enrolled in Managed Care. This is becoming such a strong method of delivery that states have chosen to manage their Medicaid populations.
Increase in Self-Directed (Participant–Directed) Care
In recent years, interest and practice in participant-directed services has increased dramatically. As of January 2022, all states now have at least one self-direction program in place, and states with self-directed programs can provide enrollees with the option to self-direct certain Medicaid services. In the self-directed model, the beneficiary chooses their caregiver and manages all day-to-day tasks. Self-Direction is an alternative method of care delivery that ensures that patients receive the care they're entitled to while still maintaining control and jurisdiction of their care plan.
However, CMS does put some guardrails in place and requires patients who self-direct to have the support from either an agency or FMS to fulfill the requirements for service plan, budget, and assistance and support for their self-directed program.
- Person-centered planning process
- Service plan
- Individualized budget
- Information and assistance in support of self-direction
The following Medicaid services may be self-directed:
- Home and Community-Based Services State Plan Option- 1915(i)
- Community First Choice-1915(k)
- Self-Directed Personal Assistance Services State Plan Option-1915(j)
- Home and Community-Based Services Waiver Programs- 1915(c)
A Shift to EVV Claims Monitoring
More than ever before, states will be actively monitoring EVV compliance in 2022. Again, the timing for claims monitoring varies by state. Some have already enacted claims penalties for non-compliant providers, and other states will be enacting a claims penalty in 2022. Courtney Martin, EVV expert at CellTrak, advises
“In 2022, I would expect that trend (claims monitoring) to continue. You'll hear the phrase soft launch, which is being used in many states. Many states are using that soft launch time to enable providers to collect and send EVV data with no impact yet to claims. When the state moves into hard launch, they'll monitor EVV compliance by providers, in one of several ways,” Martin suggests.
These ways range from simply attesting (The honor system), auditing, requiring a certain percentage of visits to include certain data, or monitoring each visit. The methods of claims monitoring currently vary by state, though trends are showing that active monitoring will be in place in 2022.
EVV to Be Required for Home Health Providers in 2023
Home Health Providers might find themselves new to EVV compliance, trying to learn the ropes, and hearing horror stories from noncompliant Medicaid providers. 2022 will be a critical year for home Health providers to prepare for the Cures Act deadline of January 1st, 2023. Our experts advise "To all the home health agencies today, is this: EVV implementation affects you now." The earlier you begin, the more time you have to perfect EVV compliance and prevent claims denial for your agency.
Final Takeaways:
Start Now – If you haven’t begun working towards EVV compliance, start now. Success with EVV takes time along with significant trial and error.
Know What Your State Requires For EVV Compliance – No two states operate the quite the same when it comes to EVV. Some states are closed and require providers to use a specific EVV vendor, others are open model, meaning you can select the vendor that’s right for your business. Attend state webinars, keep communication open with your state Payers and MCOs. Of course, CellTrak is always here to assist providers with questions they may have about EVV. Contact us at evvinfo@celltrak.com
For more information and insights from our EVV experts, check out our recent webinar with home care mogul Scott Brashears and EVV expert Courtney Martin.

